Abstract
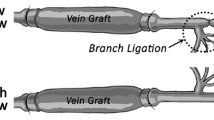
Mechanical tensile stress in vein grafts increases suddenly under the influence of arterial blood pressure. In this study, we examined the influence of increased tensile stress on the organization of the smooth muscle cells (SMCs) in the neointima and media of the rat vein grafts. An autogenous jugular vein was grafted into the abdominal aorta of the rat, and changes in the organization of the vein graft SMCs were studied by observing the distribution of SMC actin filaments and nuclei at 3 min and 1, 5, 10, and 30 days after surgery. In a normal jugular vein, the average wall circumferential tensile stress was ~ 3 kPa at an internal pressure of 3 mm Hg. The SMCs, that contained long, slender actin filamentous bundles, were oriented mainly in the circumferential direction of the vessel, and constituted a 2- to 3-cell-thick medial layer underneath the endothelium. In a vein graft, the wall circumferential tensile stress suddenly increased by ~ 140 times compared with the control level. In response to this suddenly increased stress, the SMC layer was stretched into a structure with scattered pores and disrupted SMC actin filamentous bundles within 3 min. This initial change was followed by a rapid reduction in the density of the SMC nuclei and actin filaments within 1 day and progressive SMC proliferation, that was associated with medial thickening and a change in the SMC orientation from 5 to 30 days. Further studies showed that a local inflation of normal jugular veins to 120 mm Hg for 3 min induced a similar change as found in the vein grafts, whereas the organization of the SMCs was not significantly changed in vein-vein grafts, that did not experience a change in tensile stress. These results suggested that increased tensile stress contributed to the initial damage of the SMCs and played a role in the regulation of medial SMC remodeling in vein grafts. © 1998 Biomedical Engineering Society.
PAC98: 8722-q, 8745-k
Similar content being viewed by others
REFERENCES
Adams, A. E., and J. R. Pringle. Staining of actin with fluorochrome-conjugated phalloidin. Meth. Enzym.194:729- 729, 1991.
Angelini, G. D., A. J. Bryan, H. M. Williams, R. Morgan, and A. C. Newby. Distention promotes platelet and leukocyte adhesion and reduces short-term patency in pig arteriovenous bypass grafts. J. Thorac. Cardiovasc. Surg.99:433-439, 1990.
Batellier, J., M. Wassef, R. Merval, M. Duriez, and A. Tedgui. Protection from atherosclerosis in vein grafts by a rigid external support. Arteriosclerosis Thrombosis13:379- 384, 1993.
Berceli, S. A., H. S. Borovetz, R. A. Sheppeck, H. H. Moosa, V. S. Warty, M. A. Armany, and I. M. Herman. Mechanisms of vein graft atherosclerosis: LDL metabolism and endothelial actin reorganization. J. Vascular Surg.13:336-47, 1991.
Boerboom, L. E., G. N. Olinger, T. Z. Liu, E. R. Rodriguez, V. J. Ferrans, and A. H. Kissebah. Histologic, morphometric, and biochemical evolution of vein grafts in nonhuman primate model. I. Sequential changes within the first three months. J. Thorac. Cardiovasc. Surg.99:97-106, 1990.
Bryan, A. J., and G. D. Angelini. The biology of saphenous vein graft occlusion: etiology and strategies for prevention. Curr. Opinion Cardiol.9:641-649, 1994.
Canver, C. C. Conduit options in coronary artery bypass surgery. Chest108:1150-1155, 1995.
Cassimeris, L., H. McNeill, and S. H. Zigmond. Chemoattractant-stimulated polymorphonuclear leukocytes contain two populations of actin filaments that differ in their spacial distributions and relative stabilities. J. Cell Biol.110:1067-1075, 1990.
Chobanian, A. V. 1989 Corcoran lecture: adaptive and maladaptive responses of the arterial wall to hypertension. Hypertension15:666-674, 1990.
Davies, P. F., and S. C. Tripathi. Mechanical stress mechanisms and the cell. An endothelial paradigm. Circ. Res.72:239-245, 1993.
Donaldson, M. C., J. A. Mannick, and A. D. Whittemore. Causes of primary graft failure after in situ saphenous vein bypass grafting. J. Vasc. Surg.15:113-118, 1992.
Fath, K. A., R. W. Alexander, and P. Delafontaine. Abdominal coarctation increases insulin-like growth factor I mRNA levels in rat aorta. Circ. Res.72:271-277, 1993.
Fung, Y. C. Biodynamics: Circulation. New York: Springer, 1984, pp. 77-157.
Fung, Y. C., and S. Q. Liu. Changes of residual strains in arteries due to hypertrophy caused by aortic constriction. Circ. Res.65:1340-1349, 1989.
Fung, Y. C. Biomechanics: Motion, Flow, Stress, and Growth. New York: Springer, 1990, pp. 499-546.
Fung, Y. C., and S. Q. Liu. Changes of zero-stress state of rat pulmonary arteries in hypoxic hypertension. J. Appl. Physiol.70:2455-2470, 1991.
Fung, Y. C., and S. Q. Liu. Determination of the mechanical properties of the different layers of blood vessels in vivo. Proc. Natl. Acad. Sci. USA92:2169-2173, 1995.
Girard, H. Arterial pressure in chick embryo. Am. J. Physiol.224:454-460, 1973.
Grondin, C. M., and J. C. Thornton. The natural history of saphenous vein grafts. In: Coronary Artery Graft Disease. Mechanisms and Prevention, edited by T. F. Luscher, M. Turina, and E. Braunwald. Berlin: Springer, 1994, pp. 3-15.
Gundry, S. R., M. Jones, T. Ishihara, and V. J. Ferrans. Intraoperative trauma to human saphenous veins: scanning electron microscopic comparison of preparation techniques. Ann. Thorac. Surg.30:40-45, 1980.
Hamet, P., V. Hadrava, U. Kruppa, and J. Tremblay. Transforming growth factor b1 expression and effect in aortic smooth muscle cells from spontaneously hypertensive rats. Hypertension17:896-901, 1991.
Hartwig, J. H. Mechanisms of actin rearrangements mediating platelet activation. J. Cell Biol.118:1421-1442, 1992.
Hoch, J. R., V. K. Stark, D. A. Hullett, and W. D. Turnipseed. Vein graft intimal hyperplasia: Leukocytes and cytokine gene expression. Surgery116:463-471, 1994.
Hu, N., and E. B. Clark. Hemodynamics of the stage 12 to stage 29 chick embryo. Circ. Res.65:1665-1670, 1989.
Jang, I. K., and V. Fuster. Mechanisms of plaque formation and occlusion in venous coronary bypass grafts. In: Coronary Artery Graft Disease. Mechanisms and Prevention, edited by T. F. Luscher, M. Turina, and E. Braunwald. Berlin: Springer, 1994, pp. 42-50.
Kohler, T. R., T. R. Kirkman, and A. W. Clowes. The effect of rigid external support on vein graft adaptation to the arterial circulation. J. Vasc. Surg.9:277-285, 1989.
Langille, B. L., J. J. K. Graham, D. Kim, and A. I. Gotlieb. Dynamics of shear-induced redistribution of F-actin in endothelial cells in vivo. Arteriosclerosis Thrombosis11:1814- 1820, 1991.
Liu, S. Q., and Y. C. Fung. Relationship between hypertension, hypertrophy, and opening angle of zero-stress state of arteries following aortic constriction. J. Biomech. Eng.111:325-335, 1989.
Liu, S. Q., and Y. C. Fung. Changes in the structure and mechanical properties of pulmonary arteries in rats exposed to cigarette smoke. Am. Rev. Respir. Dis.148:768-777, 1993.
Liu, S. Q., and Y. C. Fung. Material coefficients of the strain energy function of pulmonary arteries in normal and cigarette smoke-exposed rats. J. Biomech.26:1261-1269, 1993.
Liu, S. Q., M. Yen, and Y. C. Fung. On measuring the third dimension of cultured endothelial cells. Proc. Natl. Acad. Sci. USA91:8782-8786, 1994.
Liu, S. Q., and Y. C. Fung. Indicial functions of arterial remodeling in response to locally altered blood pressure. Am. J. Physiol.270:H1323-H1333, 1996.
Liu, S. Q. Vein graft engineering. In: Advances in Bioengineering, ASME Proceedings, 1996, Vol. 33, pp. 473-474.
Liu, S. Q. Alterations in structure of elastic laminae of rat pulmonary arteries in hypoxic hypertension. J. Appl. Physiol.81:2147-2155, 1996.
Liu, S. Q. Regression of hypoxic hypertension-induced changes in elastic laminae of rat pulmonary arteries. J. Appl. Physiol.82:1677–1684, 1997.
Lyall, F., M. R. Deehan, I. A. Greer, F. Boswell, W. C. Brown, and G. T. McInners. Mechanical stretch increases proto-oncogene expression and phosphoinositide turnover in vascular smooth muscle cells. J. Hypert.12:1139-1145, 1994.
Metcalfe, M. J., G. Y. Lip, and H. J. Dargie. Factors influencing coronary artery bypass graft patency. Cardiovasc. Surg.2:679-85, 1994.
Mills, N. L., and C. T. Everson. Vein graft failure. Curr. Opinion Cardiology10:562-568, 1995.
Owens, G. K. Regulation of differentiation of vascular smooth muscle cells. Physiol. Rev.75:487-517, 1995.
Sarzani, R., G. Arnaldi, and A. V. Chobanian. Hypertensioninduced changes of platelet-derived growth factor receptor expression in rat aorta and heart. Hypertension17:888-895, 1991.
Small, J. V. Organization of actin in the leading edge of cultured cells: influence of osmium tetroxide and dehydration on the ultrastructure of actin meshworks. J. Cell Biol.91:694-694, 1981.
Sumpio, B. E., A. J. Banes, M. Buckley, and G. Johnson, Jr. Alterations in aortic endothelial cell morphology and cytoskeletal protein synthesis during cyclic tensional deformation. J. Vasc. Surg.7:130-138, 1988.
Theriot, J. A. Regulation of the actin cytoskeleton in living cells. Seminars Cell Biol.5:193-199, 1994.
Zar, J. H. Biostatistical Analysis. 2nd ed. Englewood Cliffs, NJ: Prentice Hall, 1984, pp. 162-184.
Zweep, H. P., S. Satoh, B. Van der Lei, W. I. L. J. Hinrichs, F. Dijk, J. Feijen, and C. R. H. Wildevuur. Degradation of a supporting prosthesis can optimize arterialization of autologous veins. Ann. Thorac. Surg.56:1117-1122, 1993.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Liu, S.Q., Fung, Y.C. Changes in the Organization of the Smooth Muscle Cells in Rat Vein Grafts. Annals of Biomedical Engineering 26, 86–95 (1998). https://doi.org/10.1114/1.52
Issue Date:
DOI: https://doi.org/10.1114/1.52