Journal Description
Antibiotics
Antibiotics
is an international, peer-reviewed, open access journal on all aspects of antibiotics, published monthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, CAPlus / SciFinder, and other databases.
- Journal Rank: JCR - Q1 (Pharmacology & Pharmacy) / CiteScore - Q1 (General Pharmacology, Toxicology and Pharmaceutics)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 13.7 days after submission; acceptance to publication is undertaken in 2.5 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
Impact Factor:
4.8 (2022);
5-Year Impact Factor:
4.9 (2022)
Latest Articles
Pseudomonas aeruginosa Infections in Patients with Severe COVID-19 in Intensive Care Units: A Retrospective Study
Antibiotics 2024, 13(5), 390; https://doi.org/10.3390/antibiotics13050390 (registering DOI) - 25 Apr 2024
Abstract
Patients hospitalized in ICUs with severe COVID-19 are at risk for developing hospital-acquired infections, especially infections caused by Pseudomonas aeruginosa. We aimed to describe the evolution of P. aeruginosa infections in ICUs at CHRU-Nancy (France) in patients with severe COVID-19 during the
[...] Read more.
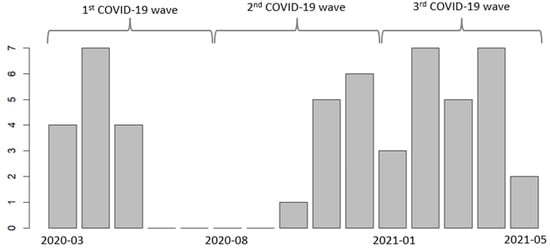
Patients hospitalized in ICUs with severe COVID-19 are at risk for developing hospital-acquired infections, especially infections caused by Pseudomonas aeruginosa. We aimed to describe the evolution of P. aeruginosa infections in ICUs at CHRU-Nancy (France) in patients with severe COVID-19 during the three initial waves of COVID-19. The second aims were to analyze P. aeruginosa resistance and to describe the antibiotic treatments. We conducted a retrospective cohort study among adult patients who were hospitalized for acute respiratory distress syndrome due to COVID-19 and who developed a hospital-acquired infection caused by P. aeruginosa during their ICU stay. Among the 51 patients included, most were male (90%) with comorbidities (77%), and the first identification of P. aeruginosa infection occurred after a median ICU stay of 11 days. Several patients acquired infections with MDR (27%) and XDR (8%) P. aeruginosa strains. The agents that strains most commonly exhibited resistance to were penicillin + β-lactamase inhibitors (59%), cephalosporins (42%), monobactams (32%), and carbapenems (27%). Probabilistic antibiotic treatment was prescribed for 49 patients (96%) and was subsequently adapted for 51% of patients after antibiogram and for 33% of patients after noncompliant antibiotic plasma concentration. Hospital-acquired infection is a common and life-threatening complication in critically ill patients. Efforts to minimize the occurrence and improve the treatment of such infections, including infections caused by resistant strains, must be pursued.
Full article
(This article belongs to the Special Issue Successful Antimicrobial Stewardship Approaches to Address Nosocomial Infections)
►
Show Figures
Open AccessArticle
Long-Term Co-Circulation of Host-Specialist and Host-Generalist Lineages of Group B Streptococcus in Brazilian Dairy Cattle with Heterogeneous Antimicrobial Resistance Profiles
by
Laura Maria Andrade de Oliveira, Leandro Correia Simões, Chiara Crestani, Natália Silva Costa, José Carlos de Figueiredo Pantoja, Renata Fernandes Rabello, Lucia Martins Teixeira, Uzma Basit Khan, Stephen Bentley, Dorota Jamrozy, Tatiana de Castro Abreu Pinto and Ruth N. Zadoks
Antibiotics 2024, 13(5), 389; https://doi.org/10.3390/antibiotics13050389 (registering DOI) - 25 Apr 2024
Abstract
Group B Streptococcus (GBS) is a major cause of contagious bovine mastitis (CBM) in Brazil. The GBS population is composed of host-generalist and host-specialist lineages, which may differ in antimicrobial resistance (AMR) and zoonotic potential, and the surveillance of bovine GBS is crucial
[...] Read more.
Group B Streptococcus (GBS) is a major cause of contagious bovine mastitis (CBM) in Brazil. The GBS population is composed of host-generalist and host-specialist lineages, which may differ in antimicrobial resistance (AMR) and zoonotic potential, and the surveillance of bovine GBS is crucial to developing effective CBM control and prevention measures. Here, we investigated bovine GBS isolates (n = 156) collected in Brazil between 1987 and 2021 using phenotypic testing and whole-genome sequencing to uncover the molecular epidemiology of bovine GBS. Clonal complex (CC) 61/67 was the predominant clade in the 20th century; however, it was replaced by CC91, with which it shares a most common recent ancestor, in the 21st century, despite the higher prevalence of AMR in CC61/67 than in CC91, and high selection pressure for AMR from indiscriminate antimicrobial use in the Brazilian dairy industry. CC103 also emerged as a dominant CC in the 21st century, and a considerable proportion of herds had two or more GBS strains, suggesting poor biosecurity and within-herd evolution due to the chronic nature of CBM problems. The majority of bovine GBS belonged to serotype Ia or III, which was strongly correlated with CCs. Ninety-three isolates were resistant to tetracycline (≥8 μg/mL; tetO = 57, tetM = 34 or both = 2) and forty-four were resistant to erythromycin (2.0 to >4 μg/mL; ermA = 1, ermB = 38, mechanism unidentified n = 5). Only three isolates were non-susceptible to penicillin (≥8.0 μg/mL), providing opportunities for improved antimicrobial stewardship through the use of narrow-spectrum antimicrobials for the treatment of dairy cattle. The common bovine GBS clades detected in this study have rarely been reported in humans, suggesting limited risk of interspecies transmission of GBS in Brazil. This study provides new data to support improvements to CBM and AMR control, bovine GBS vaccine design, and the management of public health risks posed by bovine GBS in Brazil.
Full article
(This article belongs to the Special Issue Antimicrobial Resistance of Pathogens Isolated from Bovine Mastitis)
►▼
Show Figures
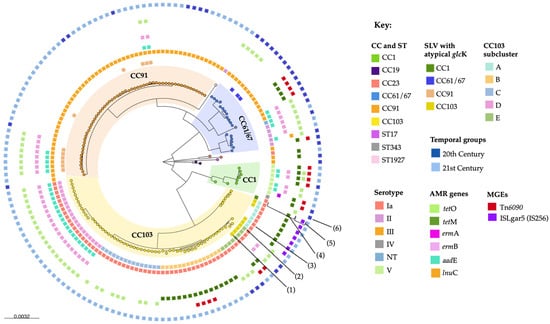
Figure 1
Open AccessArticle
Factors Associated with Prolonged Antibiotic Therapy in Neonates with Suspected Early-Onset Sepsis
by
Bo M. van der Weijden, Jolien R. van Dorth, Niek B. Achten and Frans B. Plötz
Antibiotics 2024, 13(5), 388; https://doi.org/10.3390/antibiotics13050388 (registering DOI) - 25 Apr 2024
Abstract
Early-onset sepsis (EOS) is a rare but profoundly serious bacterial infection. Neonates at risk of EOS are often treated with antibiotics. The start of empiric antibiotic therapy can successfully be reduced by the implementation of the EOS calculator. However, once started, antibiotic therapy
[...] Read more.
Early-onset sepsis (EOS) is a rare but profoundly serious bacterial infection. Neonates at risk of EOS are often treated with antibiotics. The start of empiric antibiotic therapy can successfully be reduced by the implementation of the EOS calculator. However, once started, antibiotic therapy is often continued despite a negative blood culture. To decrease the burden of antibiotic therapy, it is necessary to know whether the clinician’s reasons are based on objective factors. Therefore, we performed a retrospective single-centre cohort study to identify the factors associated with prolongation of antibiotic therapy in neonates with suspected EOS but a negative blood culture. Maternal, clinical, and laboratory data of neonates with a gestational age of ≥32 weeks, admitted between January 2019 and June 2021, were collected. Among neonates with a negative blood culture, we compared neonates with prolonged (≥3 days) to neonates with discontinued (<3 days) antibiotic therapy. The clinician’s reported reasons for prolonging therapy were explored. Blood cultures were positive in 4/146 (2.7%), negative in 131/146 (89.7%), and not obtained in 11/146 (7.5%) of the neonates. The incidence of EOS was 0.7 per 1000 neonates. Of the 131 neonates with a negative blood culture, 47 neonates (35.9%) received prolonged antibiotic therapy. In the prolonged group, the mean gestational age was higher (38.9 versus 36.8 weeks), and spontaneous preterm birth was less prevalent (21.3% versus 53.6%). Prolonged treatment was associated with late onset of respiratory distress, respiratory rate, hypoxia, apnoea and bradycardia, pale appearance, behavioural change, and elevated CRP levels. The most reported reasons were clinical appearance (38.3%), elevated CRP levels (36.2%), and skin colour (10.6%). Prolonging empiric antibiotic therapy despite a negative blood culture is common in suspected EOS. Clinical signs associated with prolongation are uncommon and the reported reasons for prolongation contain subjective assessments and arbitrary interpretations that are not supported by the guideline recommendations as arguments for prolonged therapy.
Full article
(This article belongs to the Special Issue Neonatal Infections: Epidemiology, Diagnostics and Antibiotic Therapeutics)
Open AccessCase Report
Cerebral Infectious Opportunistic Lesions in a Patient with Acute Myeloid Leukaemia: The Challenge of Diagnosis and Clinical Management
by
Gabriele Cavazza, Cristina Motto, Caroline Regna-Gladin, Giovanna Travi, Elisa Di Gennaro, Francesco Peracchi, Bianca Monti, Nicolò Corti, Rosa Greco, Periana Minga, Marta Riva, Sara Rimoldi, Marta Vecchi, Carlotta Rogati, Davide Motta, Annamaria Pazzi, Chiara Vismara, Laura Bandiera, Fulvio Crippa, Valentina Mancini, Maria Sessa, Chiara Oltolini, Roberto Cairoli and Massimo Puotiadd
Show full author list
remove
Hide full author list
Antibiotics 2024, 13(5), 387; https://doi.org/10.3390/antibiotics13050387 (registering DOI) - 24 Apr 2024
Abstract
Central nervous system (CNS) lesions, especially invasive fungal diseases (IFDs), in immunocompromised patients pose a great challenge in diagnosis and treatment. We report the case of a 48-year-old man with acute myeloid leukaemia and probable pulmonary aspergillosis, who developed hyposthenia of the left
[...] Read more.
Central nervous system (CNS) lesions, especially invasive fungal diseases (IFDs), in immunocompromised patients pose a great challenge in diagnosis and treatment. We report the case of a 48-year-old man with acute myeloid leukaemia and probable pulmonary aspergillosis, who developed hyposthenia of the left upper limb, after achieving leukaemia remission and while on voriconazole. Magnetic resonance imaging (MRI) showed oedematous CNS lesions with a haemorrhagic component in the right hemisphere with lepto-meningitis. After 2 weeks of antibiotics and amphotericin-B, brain biopsy revealed chronic inflammation with abscess and necrosis, while cultures were negative. Clinical recovery was attained, he was discharged on isavuconazole and allogeneic transplant was postponed, introducing azacitidine as a maintenance therapy. After initial improvement, MRI worsened; brain biopsy was repeated, showing similar histology; and 16S metagenomics sequencing analysis was positive (Veilonella, Pseudomonas). Despite 1 month of meropenem, MRI did not improve. The computer tomography and PET scan excluded extra-cranial infectious–inflammatory sites, and auto-immune genesis (sarcoidosis, histiocytosis, CNS vasculitis) was deemed unlikely due to the histological findings and unilateral lesions. We hypothesised possible IFD with peri-lesion inflammation and methyl-prednisolone was successfully introduced. Steroid tapering is ongoing and isavuconazole discontinuation is planned with close follow-up. In conclusion, the management of CNS complications in immunocompromised patients needs an interdisciplinary approach.
Full article
(This article belongs to the Special Issue Antimicrobial Treatment and Management of Central Nervous System Infections)
►▼
Show Figures
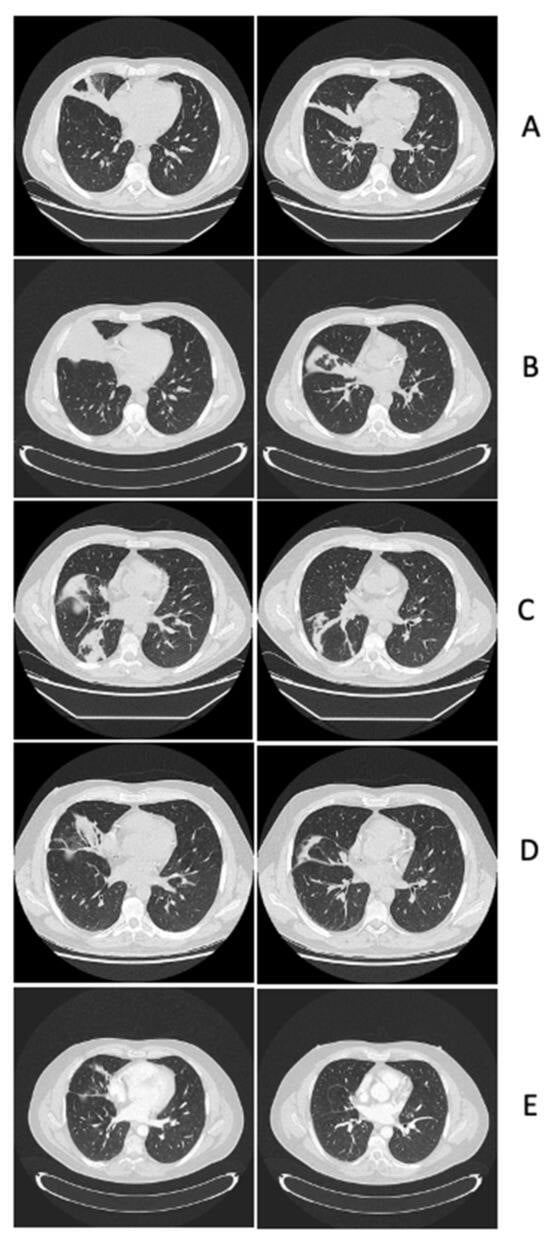
Figure 1
Open AccessArticle
Efficacy of Tamoxifen Metabolites in Combination with Colistin and Tigecycline in Experimental Murine Models of Escherichia coli and Acinetobacter baumannii
by
Soraya Herrera-Espejo, Andrea Vila-Domínguez, Tania Cebrero-Cangueiro, Younes Smani, Jerónimo Pachón, Manuel E. Jiménez-Mejías and María E. Pachón-Ibáñez
Antibiotics 2024, 13(5), 386; https://doi.org/10.3390/antibiotics13050386 - 24 Apr 2024
Abstract
This study aimed to evaluate the potential of tamoxifen and N-desmethyltamoxifen metabolites as therapeutic agents against multidrug-resistant Escherichia coli and Acinetobacter baumannii, using a repurposing approach to shorten the time required to obtain a new effective treatment against multidrug-resistant bacterial infections. Characterisation and
[...] Read more.
This study aimed to evaluate the potential of tamoxifen and N-desmethyltamoxifen metabolites as therapeutic agents against multidrug-resistant Escherichia coli and Acinetobacter baumannii, using a repurposing approach to shorten the time required to obtain a new effective treatment against multidrug-resistant bacterial infections. Characterisation and virulence studies were conducted on E. coli (colistin-susceptible C1-7-LE and colistin-resistant MCR-1+) and A. baumannii (tigecycline-susceptible Ab#9 and tigecycline-resistant Ab#186) strains. The efficacy of the metabolite mix (33.3% each) and N-desmethyltamoxifen in combination with colistimethate sodium (CMS) or tigecycline was evaluated in experimental models in mice. In the pneumonia model, N-desmethyltamoxifen exhibited significant efficacy against Ab#9 and both E. coli strains, especially E. coli MCR-1+ (−2.86 log10 CFU/g lungs, −5.88 log10 CFU/mL blood, and −50% mortality), and against the Ab#186 strain when combined with CMS (−2.27 log10 CFU/g lungs, −2.73 log10 CFU/mL blood, and −40% mortality) or tigecycline (−3.27 log10 CFU/g lungs, −4.95 log10 CFU/mL blood, and −50% mortality). Moreover, the metabolite mix in combination with both antibiotics decreased the bacterial concentrations in the lungs and blood for both A. baumannii strains. In the sepsis model, the significant efficacy of the metabolite mix was restricted to the colistin-susceptible E. coli C1-7-LE strain (−3.32 log10 CFU/g lung, −6.06 log10 CFU/mL blood, and −79% mortality). N-desmethyltamoxifen could be a new therapeutic option in combination with CMS or tigecycline for combating multidrug-resistant GNB, specifically A. baumannii.
Full article
(This article belongs to the Special Issue Advancing the Discovery and Development of New Antibiotics through Drug Repurposing)
Open AccessArticle
Use of the Naturally Occurring Bacteriophage Grouping Model for the Design of Potent Therapeutic Cocktails
by
Tea Glonti, Michael Goossens, Christel Cochez, Sabrina Green, Sayali Gorivale, Jeroen Wagemans, Rob Lavigne and Jean-Paul Pirnay
Antibiotics 2024, 13(5), 385; https://doi.org/10.3390/antibiotics13050385 - 24 Apr 2024
Abstract
The specificity of phages and their ability to evolve and overcome bacterial resistance make them potentially useful as adjuncts in the treatment of antibiotic-resistant bacterial infections. The goal of this study was to mimic a natural grouping of phages of interest and to
[...] Read more.
The specificity of phages and their ability to evolve and overcome bacterial resistance make them potentially useful as adjuncts in the treatment of antibiotic-resistant bacterial infections. The goal of this study was to mimic a natural grouping of phages of interest and to evaluate the nature of their proliferation dynamics with bacteria. We have, for the first time, transferred naturally occurring phage groups directly from their sources of isolation to in vitro and identified 13 P. aeruginosa and 11 K. pneumoniae phages of 18 different genera, whose host range was grouped as 1.2–17%, 28–48% and 60–87%, using a large collection of P. aeruginosa (n = 102) and K. pneumoniae (n = 155) strains carrying different virulence factors and phage binding receptors. We introduced the interpretation model curve for phage liquid culturing, which allows easy and quick analysis of bacterial and phage co-proliferation and growth of phage-resistant mutants (PRM) based on qualitative and partially quantitative evaluations. We assayed phage lytic activities both individually and in 14 different cocktails on planktonic bacterial cultures, including three resistotypes of P. aeruginosa (PAO1, PA14 and PA7) and seven K. pneumoniae strains of different capsular serotypes. Based on the results, the natural phage cocktails designed and tested in this study largely performed well and inhibited PRM growth either synergistically or in proto-cooperation. This study contributes to the knowledge of phage behavior in cocktails and the formulation of therapeutic phage preparations. The paper also provides a detailed description of the methods of working with phages.
Full article
(This article belongs to the Special Issue Bacteriophages and Other Alternative Antimicrobials to Combat Multidrug Resistance)
►▼
Show Figures
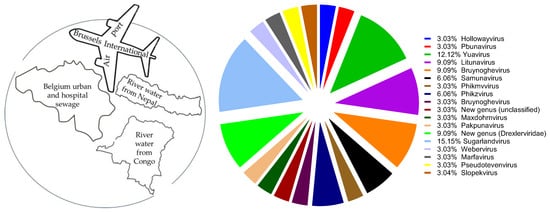
Figure 1
Open AccessEditorial
Bacterial and Fungal Pathogens: New Weapons to Fight Them
by
Charlotte A. Huber
Antibiotics 2024, 13(5), 384; https://doi.org/10.3390/antibiotics13050384 - 24 Apr 2024
Abstract
In high-income countries, degenerative diseases are the primary cause of death [...]
Full article
(This article belongs to the Special Issue Molecular Methods in Antibiotics Discovery)
Open AccessArticle
Association between Empirical Anti-Pseudomonal Antibiotics and Progression to Thoracic Surgery and Death in Empyema: Database Research
by
Akihiro Shiroshita, Kentaro Tochitani, Yohei Maki, Takero Terayama and Yuki Kataoka
Antibiotics 2024, 13(5), 383; https://doi.org/10.3390/antibiotics13050383 - 24 Apr 2024
Abstract
Evidence on the optimal antibiotic strategy for empyema is lacking. Our database study aimed to evaluate the effectiveness of empirical anti-pseudomonal antibiotics in patients with empyema. We utilised a Japanese real-world data database, focusing on patients aged ≥40 diagnosed with empyema, who underwent
[...] Read more.
Evidence on the optimal antibiotic strategy for empyema is lacking. Our database study aimed to evaluate the effectiveness of empirical anti-pseudomonal antibiotics in patients with empyema. We utilised a Japanese real-world data database, focusing on patients aged ≥40 diagnosed with empyema, who underwent thoracostomy and received intravenous antibiotics either upon admission or the following day. Patients administered intravenous vasopressors were excluded. We compared thoracic surgery and death within 90 days after admission between patients treated with empirical anti-pseudomonal and non-anti-pseudomonal antibiotics. Cause-specific hazard ratios for thoracic surgery and death were estimated using Cox proportional hazards models, with adjustment for clinically important confounders. Subgroup analyses entailed the same procedures for patients exhibiting at least one risk factor for multidrug-resistant organisms. Between March 2014 and March 2023, 855 patients with empyema meeting the inclusion criteria were enrolled. Among them, 271 (31.7%) patients received anti-pseudomonal antibiotics. The Cox proportional hazards models indicated that compared to empirical non-anti-pseudomonal antibiotics, empirical anti-pseudomonal antibiotics were associated with higher HRs for thoracic surgery and death within 90 days, respectively. Thus, regardless of the risks of multidrug-resistant organisms, empirical anti-pseudomonal antibiotics did not extend the time to thoracic surgery or death within 90 days.
Full article
(This article belongs to the Special Issue Antimicrobial Treatment of Lower Respiratory Tract Infections)
►▼
Show Figures
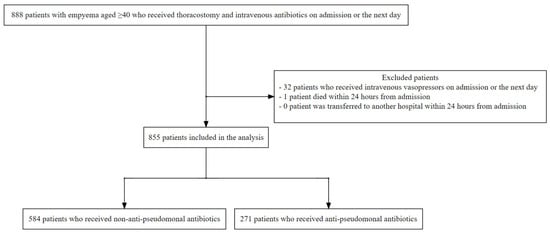
Figure 1
Open AccessArticle
Online-Assisted Survey on Antibiotic Use by Pet Owners in Dogs and Cats
by
Clara Rocholl, Yury Zablotski and Bianka Schulz
Antibiotics 2024, 13(5), 382; https://doi.org/10.3390/antibiotics13050382 - 24 Apr 2024
Abstract
The aim of the study was two-fold: first, to collect data on the use of antibiotics in Germany for dogs and cats and, second, their owners’ experiences and opinions. Using an anonymous online survey, dog and cat owners were asked about the last
[...] Read more.
The aim of the study was two-fold: first, to collect data on the use of antibiotics in Germany for dogs and cats and, second, their owners’ experiences and opinions. Using an anonymous online survey, dog and cat owners were asked about the last antibiotic administration in their pet. The inclusion criterion was any antibiotic administration within the last year. A total of 708 questionnaires from 463 dogs and 245 cats could be evaluated. Diarrhea was reported as the most common reason for antibiotic administration in dogs (18.4%). Wound infection/abscess/bite injury was the second most common reason in dogs (16.0%). In cats wound infection/abscess/bite injury was the most common reason (23.3%), followed by dental treatment (21.2%) and upper respiratory tract infections (16.7%). The most common antibiotics used systemically in both species were amoxicillin/clavulanic acid (32.5%), amoxicillin (14.8%), metronidazole (6.9%), and doxycycline (6.8%). While efficacy (99.9%) and tolerability (94.8%) were rated as most important for the choice of antibiotics, costs (51.6%) were cited as predominantly unimportant. First-line antibiotics were used significantly more often than critically important antibiotics. The majority of animal owners show awareness for avoidance of antibiotic resistance and the use of critically important antibiotics.
Full article
(This article belongs to the Section Antibiotics in Animal Health)
►▼
Show Figures
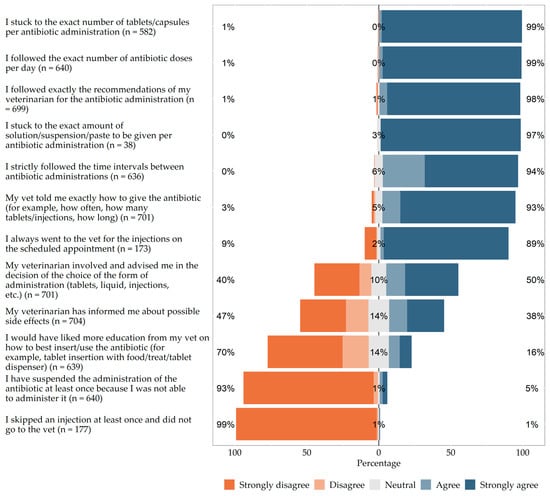
Figure 1
Open AccessArticle
Multidrug-Resistant Escherichia coli Remains Susceptible to Metal Ions and Graphene-Based Compounds
by
Nathalie Karaky, Shiying Tang, Parameshwari Ramalingam, Andrew Kirby, Andrew J. McBain, Craig E. Banks and Kathryn A. Whitehead
Antibiotics 2024, 13(5), 381; https://doi.org/10.3390/antibiotics13050381 - 24 Apr 2024
Abstract
Escherichia coli is listed as a priority 1 pathogen on the World Health Organization (WHO) priority pathogen list. For this list of pathogens, new antibiotics are urgently needed to control the emergence and spread of multidrug-resistant strains. This study assessed eighteen metal ions, graphene,
[...] Read more.
Escherichia coli is listed as a priority 1 pathogen on the World Health Organization (WHO) priority pathogen list. For this list of pathogens, new antibiotics are urgently needed to control the emergence and spread of multidrug-resistant strains. This study assessed eighteen metal ions, graphene, and graphene oxide for their antimicrobial efficacy against E. coli in both planktonic and biofilm growth states and the potential synergy between metal ions and graphene-based compounds. Molybdenum and tin ions exhibited the greatest antimicrobial activity against the planktonic states of the isolates with minimal inhibitory concentrations (MIC) ranging between 13 mg/L and 15.6 mg/L. Graphene oxide had no antimicrobial effect against any of the isolates, while graphene showed a moderate effect against E. coli (MIC, 62.5 mg/L). Combinations of metal ions and graphene-based compounds including tin–graphene, tin–graphene oxide, gold–graphene, platinum–graphene, and platinum–graphene oxide exhibited a synergistic antimicrobial effect (FIC ≤ 0.5), inhibiting the planktonic and biofilm formation of the isolates regardless of their antibiotic-resistant profiles. The bactericidal effect of the metal ions and the synergistic effects when combined with graphene/graphene oxide against medically relevant pathogens demonstrated that the antimicrobial efficacy was increased. Hence, such agents may potentially be used in the production of novel antimicrobial/antiseptic agents.
Full article
(This article belongs to the Special Issue Antibiotic Adjuvants: An Approach to Overcoming Multi-Drug Resistance and Biofilm Infections)
►▼
Show Figures
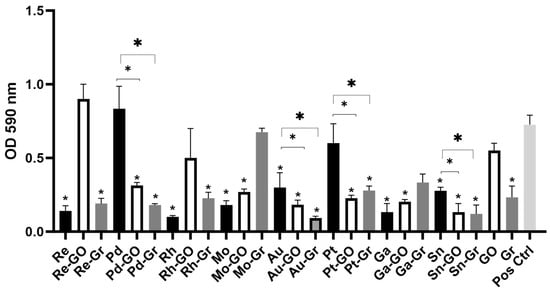
Figure 1
Open AccessArticle
Camel Milk Resistome in Kuwait: Genotypic and Phenotypic Characterization
by
Rita Rahmeh, Abrar Akbar, Batlah Almutairi, Mohamed Kishk, Naida Babic Jordamovic, Abdulaziz Al-Ateeqi, Anisha Shajan, Heba Al-Sherif, Alfonso Esposito, Sabah Al-Momin and Silvano Piazza
Antibiotics 2024, 13(5), 380; https://doi.org/10.3390/antibiotics13050380 - 23 Apr 2024
Abstract
Antimicrobial resistance (AMR) is one of the major global health and economic threats. There is growing concern about the emergence of AMR in food and the possibility of transmission of microorganisms possessing antibiotic resistance genes (ARGs) to the human gut microbiome. Shotgun sequencing
[...] Read more.
Antimicrobial resistance (AMR) is one of the major global health and economic threats. There is growing concern about the emergence of AMR in food and the possibility of transmission of microorganisms possessing antibiotic resistance genes (ARGs) to the human gut microbiome. Shotgun sequencing and in vitro antimicrobial susceptibility testing were used in this study to provide a detailed characterization of the antibiotic resistance profile of bacteria and their ARGs in dromedary camel milk. Eight pooled camel milk samples, representative of multiple camels distributed in the Kuwait desert, were collected from retail stores and analyzed. The genotypic analysis showed the presence of ARGs that mediate resistance to 18 classes of antibiotics in camel milk, with the highest resistance to fluoroquinolones (12.48%) and disinfecting agents and antiseptics (9%). Furthermore, the results pointed out the possible transmission of the ARGs to other bacteria through mobile genetic elements. The in vitro antimicrobial susceptibility testing indicated that 80% of the isolates were resistant to different classes of antibiotics, with the highest resistance observed against three antibiotic classes: penicillin, tetracyclines, and carbapenems. Multidrug-resistant pathogens including Klebsiella pneumoniae, Escherichia coli, and Enterobacter hormaechei were also revealed. These findings emphasize the human health risks related to the handling and consumption of raw camel milk and highlight the necessity of improving the hygienic practices of farms and retail stores to control the prevalence of ARGs and their transmission.
Full article
(This article belongs to the Special Issue Antimicrobial Resistance in Animals and Animal Products and Its Environmental Transmission Aspects)
►▼
Show Figures
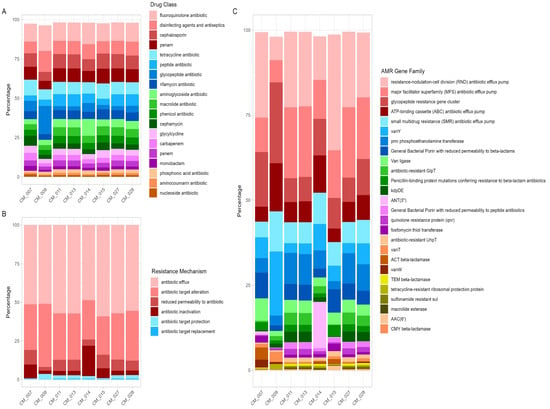
Figure 1
Open AccessArticle
First Insights on Resistance and Virulence Potential of Escherichia coli from Captive Birds of Prey in Portugal
by
Rita Magalhães, Raquel Abreu, Gonçalo Pereira, Eva Cunha, Elisabete Silva, Luís Tavares, Lélia Chambel and Manuela Oliveira
Antibiotics 2024, 13(5), 379; https://doi.org/10.3390/antibiotics13050379 - 23 Apr 2024
Abstract
Captive birds of prey are often used for pest control in urban areas, while also participating in falconry exhibitions. Traveling across the country, these birds may represent a public health concern as they can host pathogenic and zoonotic agents and share the same
[...] Read more.
Captive birds of prey are often used for pest control in urban areas, while also participating in falconry exhibitions. Traveling across the country, these birds may represent a public health concern as they can host pathogenic and zoonotic agents and share the same environment as humans and synanthropic species. In this work, Escherichia coli from the cloacal samples of 27 captive birds of prey were characterized to determine their pathogenic potential. Isolates were clustered through ERIC-PCR fingerprinting, and the phylogenetic groups were assessed using a quadruplex PCR method. Their virulence and resistance profile against nine antibiotics were determined, as well as the isolates’ ability to produce extended-spectrum β-lactamases (ESBLs). The 84 original isolates were grouped into 33 clonal types, and it was observed that more than half of the studied isolates belonged to groups D and B2. Most isolates presented gelatinase activity (88%), almost half were able to produce biofilm (45%), and some were able to produce α-hemolysin (18%). The isolates presented high resistance rates towards piperacillin (42%), tetracycline (33%), and doxycycline (30%), and 6% of the isolates were able to produce ESBLs. The results confirm the importance of these birds as reservoirs of virulence and resistance determinants that can be disseminated between wildlife and humans, stressing the need for more studies focusing on these animals.
Full article
(This article belongs to the Special Issue Antimicrobial Resistance and Virulence in Veterinary Pathogens)
►▼
Show Figures
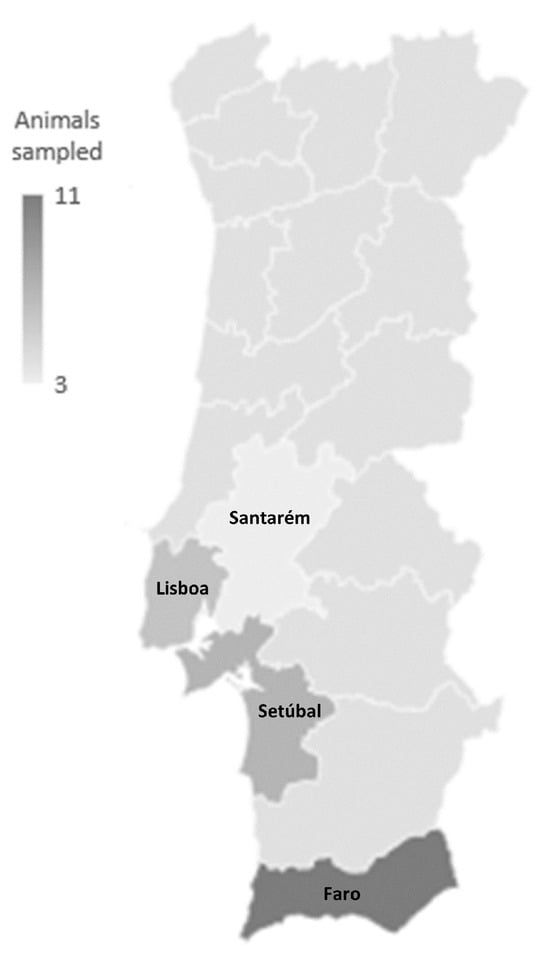
Figure 1
Open AccessArticle
Incidence, Outcomes, and Risk Factors for Isoniazid-Resistant Tuberculosis from 2012 to 2022 in Eastern China
by
Yan Shao, Wenlei Song, Honghuan Song, Guoli Li, Limei Zhu, Qiao Liu and Cheng Chen
Antibiotics 2024, 13(4), 378; https://doi.org/10.3390/antibiotics13040378 - 22 Apr 2024
Abstract
Background: Isoniazid-resistant, rifampicin-susceptible tuberculosis (Hr-TB) is the most frequent drug-resistant tuberculosis (DR-TB) in the world, and unfavorable outcomes of Hr-TB are more common compared to drug-susceptible TB. Considering there is no optimal regimen accepted worldwide, we undertook a retrospective cohort study in eastern
[...] Read more.
Background: Isoniazid-resistant, rifampicin-susceptible tuberculosis (Hr-TB) is the most frequent drug-resistant tuberculosis (DR-TB) in the world, and unfavorable outcomes of Hr-TB are more common compared to drug-susceptible TB. Considering there is no optimal regimen accepted worldwide, we undertook a retrospective cohort study in eastern China to estimate incidence trends and risk factors associated with unfavorable outcomes of Hr-TB. Methods: Between January 2012 and December 2022, all Hr-TB patients’ information was extracted from the Tuberculosis Information Management System (TIMS), which is a national electronic information platform, to record TB patients’ clinical information in this study. The incidence of Hr-TB was determined by the mid-year population according to census data published by the government. We categorized treatment regimens depending on fluoroquinolone (FQ) use, and potential risk factors were analyzed using multivariable logistic regression. Results: A total of 3116 Hr-TB patients fulfilled the inclusion criteria and were enrolled in this study. The average annual rate of Hr-TB in the 11 years under investigation was 0.34 per 100,000 and increased to 0.53 per 100,000 until 2019. In total, six different treatment regimens were utilized in the study sites, and less than 1% of regimens adopted FQ. There was no difference in the unfavorable outcomes between the FQ-included and FQ-excluded groups (p = 0.22). The average treatment duration was 7.06 months, and the longest treatment was 26 months. Approximately 20% (637/3116) of Hr-TB patients had unfavorable outcomes, and 60.13% (383/637) of them proceeded to multidrug-resistant tuberculosis (MDR-TB). Treatment duration and a positive smear at the end of the 5th month were significantly associated with unfavorable outcomes (p < 0.001). Conclusion: The unfavorable treatment outcomes of Hr-TB are still high in eastern China, and the efficacy of FQ-containing regimens needs to be validated for Hr-TB treatment.
Full article
(This article belongs to the Special Issue Tuberculosis: Mycobacterium tuberculosis—Infection Control and Antibiotic Resistance)
►▼
Show Figures
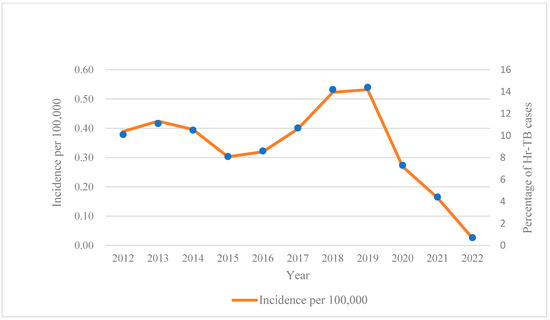
Figure 1
Open AccessArticle
The Epidemiology, Management and Therapeutic Outcomes of Subdural Empyema in Neonates with Acute Bacterial Meningitis
by
Wei-Ju Lee, Ming-Horng Tsai, Jen-Fu Hsu, Shih-Ming Chu, Chih-Chen Chen, Peng-Hong Yang, Hsuan-Rong Huang, Miao-Ching Chi, Chiang-Wen Lee and Mei-Chen Ou-Yang
Antibiotics 2024, 13(4), 377; https://doi.org/10.3390/antibiotics13040377 - 21 Apr 2024
Abstract
►▼
Show Figures
Background: Subdural empyema is one of the more serious complications of bacterial meningitis and therapeutic challenges to clinicians. We aimed to evaluate the clinical characteristics, treatment, and outcome of subdural empyema in neonates with bacterial meningitis. Methods: A retrospective cohort study was conducted
[...] Read more.
Background: Subdural empyema is one of the more serious complications of bacterial meningitis and therapeutic challenges to clinicians. We aimed to evaluate the clinical characteristics, treatment, and outcome of subdural empyema in neonates with bacterial meningitis. Methods: A retrospective cohort study was conducted in two medical centers in Taiwan that enrolled all cases of neonates with subdural empyema after bacterial meningitis between 2003 and 2020. Results: Subdural empyema was diagnosed in 27 of 153 (17.6%) neonates with acute bacterial meningitis compared with cases of meningitis without subdural empyema. The demographics and pathogen distributions were comparable between the study group and the controls, but neonates with subdural empyema were significantly more likely to have clinical manifestations of fever (85.2%) and seizure (81.5%) (both p values < 0.05). The cerebrospinal fluid results of neonates with subdural empyema showed significantly higher white blood cell counts, lower glucose levels and higher protein levels (p = 0.011, 0.003 and 0.006, respectively). Neonates with subdural empyema had a significantly higher rate of neurological complications, especially subdural effusions and periventricular leukomalacia. Although the final mortality rate was not increased in neonates with subdural empyema when compared with the controls, they were often treated much longer and had a high rate of long-term neurological sequelae. Conclusions: Subdural empyema is not uncommon in neonates with acute bacterial meningitis and was associated with a high risk of neurological complications, although it does not significantly increase the final mortality rate. Close monitoring of the occurrence of subdural empyema is required, and appropriate long-term antibiotic treatment after surgical intervention may lead to optimized outcomes.
Full article
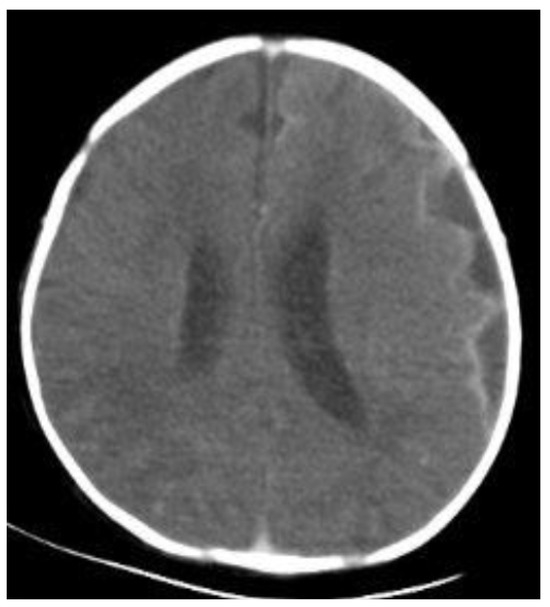
Figure 1
Open AccessArticle
Rabbits as a Reservoir of Multidrug-Resistant Escherichia coli: Clonal Lineages and Public Health Impact
by
Adriana Silva, Vanessa Silva, Teresa Tavares, María López, Beatriz Rojo-Bezares, José Eduardo Pereira, Virgílio Falco, Patrícia Valentão, Gilberto Igrejas, Yolanda Sáenz and Patrícia Poeta
Antibiotics 2024, 13(4), 376; https://doi.org/10.3390/antibiotics13040376 - 20 Apr 2024
Abstract
Escherichia coli, including extended-spectrum β-lactamases (ESBL)-producing strains, poses a global health threat due to multidrug resistance, compromising food safety and environmental integrity. In industrial settings, rabbits raised for meat have the highest consumption of antimicrobial agents compared to other food-producing animals. The
[...] Read more.
Escherichia coli, including extended-spectrum β-lactamases (ESBL)-producing strains, poses a global health threat due to multidrug resistance, compromising food safety and environmental integrity. In industrial settings, rabbits raised for meat have the highest consumption of antimicrobial agents compared to other food-producing animals. The European Union is facing challenges in rabbit farming as rabbit consumption declines and antibiotic-resistant strains of E. coli cause enteric diseases. The aim of this study was to investigate the antibiotic resistance profile, genetic diversity, and biofilm formation in cefotaxime-resistant E. coli strains isolated from twenty rabbit farms in Northern Portugal to address the effect of the pressing issue of antibiotic resistance in the rabbit farming industry. Resistance to critically antibiotics was observed, with high levels of resistance to several categories, such as tetracycline, ampicillin, aztreonam, and streptomycin. However, all isolates were susceptible to cefoxitin and imipenem. Multidrug resistance was common, with strains showing resistance to all antibiotics tested. The blaCTX-M variants (blaCTX-3G and blaCTX-M9), followed by the tetracycline resistance genes, were the most frequent resistance genes found. ST10 clones exhibiting significant resistance to various categories of antibiotics and harboring different resistance genes were detected. ST457 and ST2325 were important sequence types due to their association with ESBL-E. coli isolates and have been widely distributed in a variety of environments and host species. The strains evaluated showed a high capacity for biofilm formation, which varied when they were grouped by the number of classes of antibiotics to which they showed resistance (i.e., seven different classes of antibiotics, six classes of antibiotics, and three/four/five classes of antibiotics). The One Health approach integrates efforts to combat antimicrobial resistance in rabbit farming through interdisciplinary collaboration of human, animal, and environmental health. Our findings are worrisome and raise concerns. The extensive usage of antibiotics in rabbit farming emphasizes the urgent need to establish active surveillance systems.
Full article
(This article belongs to the Special Issue Zoonotic Diseases: Pathogen Detection and Antimicrobial Treatment)
►▼
Show Figures
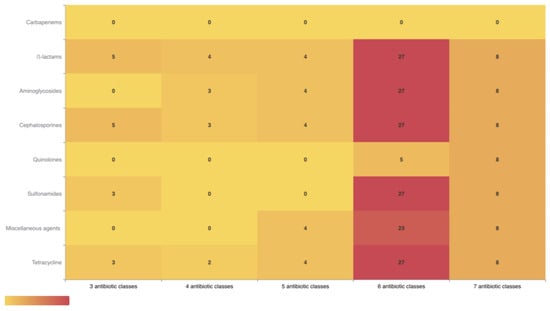
Figure 1
Open AccessReview
Antimicrobial De-Escalation in Critically Ill Patients
by
Eloisa Sofia Tanzarella, Salvatore Lucio Cutuli, Gianmarco Lombardi, Fabiola Cammarota, Alessandro Caroli, Emanuele Franchini, Elena Sancho Ferrando, Domenico Luca Grieco, Massimo Antonelli and Gennaro De Pascale
Antibiotics 2024, 13(4), 375; https://doi.org/10.3390/antibiotics13040375 - 19 Apr 2024
Abstract
Antimicrobial de-escalation (ADE) is defined as the discontinuation of one or more antimicrobials in empirical therapy, or the replacement of a broad-spectrum antimicrobial with a narrower-spectrum antimicrobial. The aim of this review is to provide an overview of the available literature on the
[...] Read more.
Antimicrobial de-escalation (ADE) is defined as the discontinuation of one or more antimicrobials in empirical therapy, or the replacement of a broad-spectrum antimicrobial with a narrower-spectrum antimicrobial. The aim of this review is to provide an overview of the available literature on the effectiveness and safety of ADE in critically ill patients, with a focus on special conditions such as anti-fungal therapy and high-risk categories. Although it is widely considered a safe strategy for antimicrobial stewardship (AMS), to date, there has been no assessment of the effect of de-escalation on the development of resistance. Conversely, some authors suggest that prolonged antibiotic treatment may be a side effect of de-escalation, especially in high-risk categories such as neutropenic critically ill patients and intra-abdominal infections (IAIs). Moreover, microbiological documentation is crucial for increasing ADE rates in critically ill patients with infections, and efforts should be focused on exploring new diagnostic tools to accelerate pathogen identification. For these reasons, ADE can be safely used in patients with infections, as confirmed by high-quality and reliable microbiological samplings, although further studies are warranted to clarify its applicability in selected populations.
Full article
(This article belongs to the Special Issue Antibacterial Resistance and Infection Control in ICU)
Open AccessArticle
Hospital Wastes as Potential Sources for Multi-Drug-Resistant ESBL-Producing Bacteria at a Tertiary Hospital in Ethiopia
by
Mulatu Gashaw, Esayas Kebede Gudina, Wondwossen Tadesse, Guenter Froeschl, Solomon Ali, Thomas Seeholzer, Arne Kroidl and Andreas Wieser
Antibiotics 2024, 13(4), 374; https://doi.org/10.3390/antibiotics13040374 - 19 Apr 2024
Abstract
►▼
Show Figures
The hospital environment is increasingly becoming an important reservoir for multi-drug-resistant (MDR) Gram-negative bacteria, posing serious challenges to efforts to combat antimicrobial resistance (AMR). This study aimed to investigate the role of hospital waste as a potential source of MDR ESBL-producing bacteria. Samples
[...] Read more.
The hospital environment is increasingly becoming an important reservoir for multi-drug-resistant (MDR) Gram-negative bacteria, posing serious challenges to efforts to combat antimicrobial resistance (AMR). This study aimed to investigate the role of hospital waste as a potential source of MDR ESBL-producing bacteria. Samples were collected from multiple sources within a hospital and its vicinity, including surface swabs, houseflies, and sewage samples. The samples were subsequently processed in a microbiology laboratory to identify potential pathogenic bacteria and confirmed using MALDI-TOF MS. Bacteria were isolated from 87% of samples, with the predominant isolates being E. coli (30.5%), Klebsiella spp. (12.4%), Providencia spp. (12.4%), and Proteus spp. (11.9%). According to the double disc synergy test (DDST) analysis, nearly half (49.2%) of the bacteria were identified as ESBL producers. However, despite exhibiting complete resistance to beta-lactam antibiotics, 11.8% of them did not test positive for ESBL production. The characterization of E. coli revealed that 30.6% and 5.6% of them carried blaCTX-M group 1 type-15 and blaNDM genes, respectively. This finding emphasizes the importance of proper hospital sanitation and waste management practices to mitigate the spread of AMR within the healthcare setting and safeguard the health of both patients and the wider community.
Full article
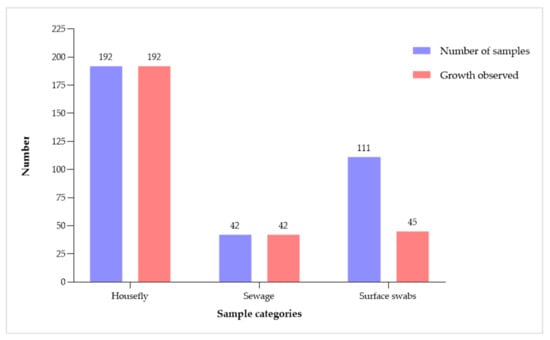
Figure 1
Open AccessArticle
No Sequestration of Commonly Used Anti-Infectives in the Extracorporeal Membrane Oxygenation (ECMO) Circuit—An Ex Vivo Study
by
Hendrik Booke, Benjamin Friedrichson, Lena Draheim, Thilo Caspar von Groote, Otto Frey, Anka Röhr, Kai Zacharowski and Elisabeth Hannah Adam
Antibiotics 2024, 13(4), 373; https://doi.org/10.3390/antibiotics13040373 - 19 Apr 2024
Abstract
Patients undergoing extracorporeal membrane oxygenation (ECMO) often require therapy with anti-infective drugs. The pharmacokinetics of these drugs may be altered during ECMO treatment due to pathophysiological changes in the drug metabolism of the critically ill and/or the ECMO therapy itself. This study investigates
[...] Read more.
Patients undergoing extracorporeal membrane oxygenation (ECMO) often require therapy with anti-infective drugs. The pharmacokinetics of these drugs may be altered during ECMO treatment due to pathophysiological changes in the drug metabolism of the critically ill and/or the ECMO therapy itself. This study investigates the latter aspect for commonly used anti-infective drugs in an ex vivo setting. A fully functional ECMO device circulated an albumin–electrolyte solution through the ECMO tubes and oxygenator. The antibiotic agents cefazolin, cefuroxim, cefepime, cefiderocol, linezolid and daptomycin and the antifungal agent anidulafungin were added. Blood samples were taken over a period of four hours and drug concentrations were measured via high-pressure liquid chromatography (HPLC) with UV detection. Subsequently, the study analyzed the time course of anti-infective concentrations. The results showed no significant changes in the concentration of any tested anti-infectives throughout the study period. This ex vivo study demonstrates that the ECMO device itself has no impact on the concentration of commonly used anti-infectives. These findings suggest that ECMO therapy does not contribute to alterations in the concentrations of anti-infective medications in severely ill patients.
Full article
(This article belongs to the Special Issue Pharmacokinetic and Antibiotic Dosing for Intensive Care Unit Patients)
►▼
Show Figures
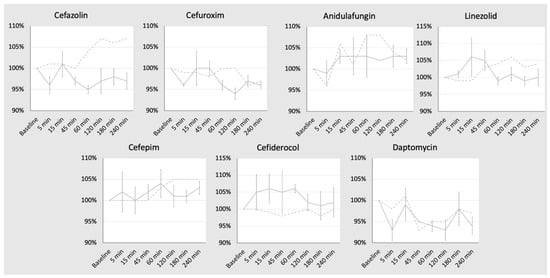
Figure 1
Open AccessArticle
Comparative Pharmacokinetics of Gentamicin C1, C1a and C2 in Healthy and Infected Piglets
by
Eun-Young Kim, Tae-Won Kim, Elias Gebru Awji, Eon-Bee Lee and Seung-Chun Park
Antibiotics 2024, 13(4), 372; https://doi.org/10.3390/antibiotics13040372 - 18 Apr 2024
Abstract
Gentamicin, an aminoglycoside antibiotic, is a mixture of therapeutically active C1, C1a, C2 and other minor components. Despite its decades-long use in pigs and other species, its intramuscular (IM) pharmacokinetics/pharmacodynamics (PKs/PDs) are unknown in piglets. Furthermore, the PKs
[...] Read more.
Gentamicin, an aminoglycoside antibiotic, is a mixture of therapeutically active C1, C1a, C2 and other minor components. Despite its decades-long use in pigs and other species, its intramuscular (IM) pharmacokinetics/pharmacodynamics (PKs/PDs) are unknown in piglets. Furthermore, the PKs of many drugs differ between healthy and sick animals. Therefore, we investigated the PKs of gentamicin after a single IM dose (10 mg/kg) in healthy piglets and piglets that were intranasally co-infected with Actinobacillus pleuropneumoniae and Pasteurella multocida (PM). The plasma concentrations were measured using validated liquid chromatography/mass spectrometry. The gentamicin exposure was 36% lower based on the area under the plasma concentration–time curve and 16% lower based on the maximum plasma concentration (Cmax) in the infected piglets compared to the healthy piglets, while it was eliminated faster (shorter half-life and larger clearance) in the infected piglets compared to the healthy piglets. The clearance and volume of distribution were the highest for the C1 component. C1, C1a and C2 accounted for 22–25%, 33–37% and 40–42% of the total gentamicin exposure, respectively. The PK/PD target for the efficacy of aminoglycosides (Cmax/minimum inhibitory concentration (MIC) > 10) could be exceeded for PM, with a greater magnitude in the healthy piglets. We suggest integrating this PK information with antibiotic susceptibility data for other bacteria to make informed antibiotic and dosage regimen selections against piglet infections.
Full article
(This article belongs to the Special Issue Rational Use of Antibiotics in Veterinary Medicine)
►▼
Show Figures
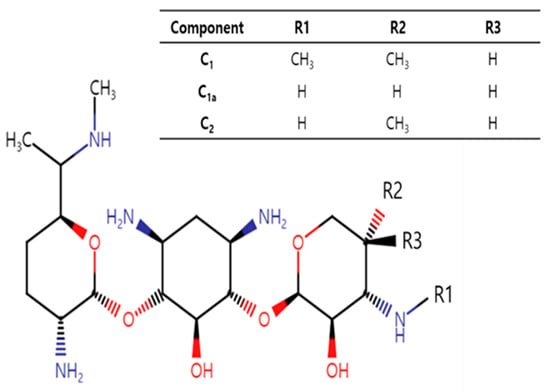
Figure 1
Open AccessArticle
Antibacterial Activity of Oregano (Origanum vulgare L.) Essential Oil Vapors against Microbial Contaminants of Food-Contact Surfaces
by
Loris Pinto, Salvatore Cervellieri, Thomas Netti, Vincenzo Lippolis and Federico Baruzzi
Antibiotics 2024, 13(4), 371; https://doi.org/10.3390/antibiotics13040371 - 18 Apr 2024
Abstract
The antimicrobial effect of eight essential oils’ vapors against pathogens and spoilage bacteria was assayed. Oreganum vulgare L. essential oil (OVO) showed a broad antibacterial effect, with Minimum Inhibitory Concentration (MIC) values ranging from 94 to 754 µg cm−3 air, depending on
[...] Read more.
The antimicrobial effect of eight essential oils’ vapors against pathogens and spoilage bacteria was assayed. Oreganum vulgare L. essential oil (OVO) showed a broad antibacterial effect, with Minimum Inhibitory Concentration (MIC) values ranging from 94 to 754 µg cm−3 air, depending on the bacterial species. Then, gaseous OVO was used for the treatment of stainless steel, polypropylene, and glass surfaces contaminated with four bacterial pathogens at 6–7 log cfu coupon−1. No viable cells were found after OVO treatment on all food-contact surfaces contaminated with all pathogens, with the exception of Sta. aureus DSM 799 on the glass surface. The antimicrobial activity of OVO after the addition of beef extract as a soiling agent reduced the Sta. aureus DSM 799 viable cell count by more than 5 log cfu coupon−1 on polypropylene and glass, while no viable cells were found in the case of stainless steel. HS-GC-MS analysis of the headspace of the boxes used for the antibacterial assay revealed 14 different volatile compounds with α-Pinene (62–63%), and p-Cymene (21%) as the main terpenes. In conclusion, gaseous OVO could be used for the microbial decontamination of food-contact surfaces, although its efficacy needs to be evaluated since it depends on several parameters such as target microorganisms, food-contact material, temperature, time of contact, and relative humidity.
Full article
(This article belongs to the Special Issue Essential Oil of the Plants: Chemical Composition, Antimicrobial Activity, and Biological Applications)
►▼
Show Figures
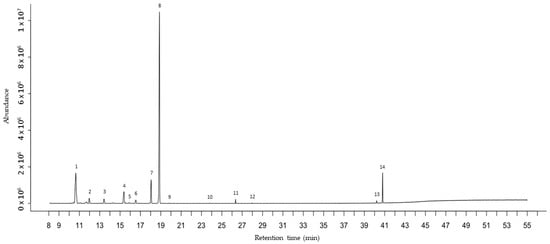
Figure 1

Journal Menu
► ▼ Journal Menu-
- Antibiotics Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Antibiotics, Antioxidants, JoF, Microbiology Research, Microorganisms
Redox in Microorganisms, 2nd Edition
Topic Editors: Michal Letek, Volker BehrendsDeadline: 31 July 2024
Topic in
Antibiotics, JPM, Pharmaceuticals, Pharmaceutics
Pharmacokinetic and Pharmacodynamic Modelling in Drug Discovery and Development
Topic Editors: Inaki F. Troconiz, Victor Mangas Sanjuán, Maria Garcia-Cremades MiraDeadline: 31 August 2024
Topic in
Molecules, Pharmaceutics, Antibiotics, Microorganisms, Biomolecules, Marine Drugs, Polymers, IJMS
Antimicrobial Agents and Nanomaterials
Topic Editors: Sandra Pinto, Vasco D. B. BonifácioDeadline: 30 September 2024
Topic in
Antibiotics, Biomedicines, JCM, Pharmaceuticals, Pharmaceutics
Challenges and Future Prospects of Antibacterial Therapy
Topic Editors: Kwang-sun Kim, Zehra EdisDeadline: 31 October 2024

Conferences
Special Issues
Special Issue in
Antibiotics
When Communities Matter: Interplay between Mobile Genetic Elements and Antibiotic Resistance
Guest Editor: Antony T. VincentDeadline: 30 April 2024
Special Issue in
Antibiotics
Antibacterial Treatment in Periodontal and Endodontic Therapy, 2nd Volume
Guest Editors: Andreas Braun, Felix KrauseDeadline: 15 May 2024
Special Issue in
Antibiotics
The Application of Antibiotic Therapy in Oral Surgery and Dental Implant Procedures
Guest Editors: Eugenio Velasco-Ortega, Angel-Orion Salgado-Peralvo, Juan Francisco Peña-CardellesDeadline: 31 May 2024
Special Issue in
Antibiotics
Challenges for Therapeutic Drug Monitoring of Antimicrobials
Guest Editors: Giuseppe Pipitone, Giuseppe Nunnari, Fabrizio TagliettiDeadline: 15 June 2024
Topical Collections
Topical Collection in
Antibiotics
Antimicrobial Resistance and Anti-Biofilms
Collection Editors: Ding-Qiang Chen, Yulong Tan, Ren-You Gan, Guanggang Qu, Zhenbo Xu, Junyan Liu