Abstract
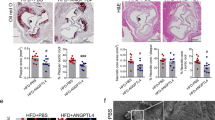
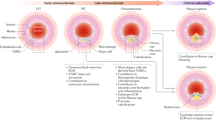
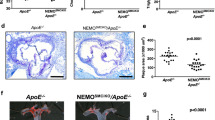
Vascular smooth muscle cell (VSMC) apoptosis occurs in many arterial diseases, including aneurysm formation, angioplasty restenosis and atherosclerosis. Although VSMC apoptosis promotes vessel remodeling, coagulation and inflammation, its precise contribution to these diseases is unknown, given that apoptosis frequently accompanies vessel injury or alterations to flow. To study the direct consequences of VSMC apoptosis, we generated transgenic mice expressing the human diphtheria toxin receptor (hDTR, encoded by HBEGF) from a minimal Tagln (also known as SM22α) promoter. Despite apoptosis inducing loss of 50–70% of VSMCs, normal arteries showed no inflammation, reactive proliferation, thrombosis, remodeling or aneurysm formation. In contrast, VSMC apoptosis in atherosclerotic plaques of SM22α-hDTR Apoe−/− mice induced marked thinning of fibrous cap, loss of collagen and matrix, accumulation of cell debris and intense intimal inflammation. We conclude that VSMC apoptosis is 'silent' in normal arteries, which have a large capacity to withstand cell loss. In contrast, VSMC apoptosis alone is sufficient to induce features of plaque vulnerability in atherosclerosis. SM22α-hDTR Apoe−/− mice may represent an important new model to test agents proposed to stabilize atherosclerotic plaques.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Lutgens, E. et al. Biphasic pattern of cell turnover characterizes the progression from fatty streaks to ruptured human atherosclerotic plaques. Cardiovasc. Res. 41, 473–479 (1999).
Geng, Y. & Libby, P. Evidence for apoptosis in advanced human atheroma: colocalization with interleukin-1β converting enzyme. Am J Pathol 147, 251–266 (1995).
Malik, N. et al. Apoptosis and cell proliferation after porcine coronary angioplasty. Circulation 98, 1657–1665 (1998).
Clowes, A.W., Reidy, M.A. & Clowes, M.M. Kinetics of cellular proliferation after arterial injury. I. Smooth muscle growth in the absence of endothelium. Lab. Invest. 49, 327–333 (1983).
LopezCandales, A. et al. Decreased vascular smooth muscle cell density in medial degeneration of human abdominal aortic aneurysms. Am. J. Pathol. 150, 993–1007 (1997).
Cho, A., Courtman, D. & Langille, L. Apoptosis (programmed cell death) in arteries of the neonatal lamb. Circ. Res. 76, 168–175 (1995).
Cho, A., Mitchell, L., Koopmans, D. & Langille, B.L. Effects of changes in blood flow rate on cell death and cell proliferation in carotid arteries of immature rabbits. Circ. Res. 81, 328–337 (1997).
Littlewood, T.D. & Bennett, M.R. Apoptotic cell death in atherosclerosis. Curr. Opin. Lipidol. 14, 469–475 (2003).
Schaub, F.J. et al. Fas and Fas-associated death domain protein regulate monocyte chemoattractant protein-1 expression by human smooth muscle cells through caspase- and calpain-dependent release of interleukin-1α. Circ. Res. 93, 515–522 (2003).
Schaub, F.J. et al. Fas/FADD-mediated activation of a specific program of inflammatory gene expression in vascular smooth muscle cells. Nat. Med. 6, 790–796 (2000).
Li, L., Miano, J.M., Mercer, B. & Olson, E.N. Expression of the SM22alpha promoter in transgenic mice provides evidence for distinct transcriptional regulatory programs in vascular and visceral smooth muscle cells. J. Cell Biol. 132, 849–859 (1996).
Naglich, J.G., Rolf, J.M. & Eidels, L. Expression of functional diphtheria toxin receptors on highly toxin-sensitive mouse cells that specifically bind radioiodinated toxin. Proc. Natl. Acad. Sci. USA 89, 2170–2174 (1992).
Chung, D.W. & Collier, R.J. The mechanism of ADP-ribosylation of elongation factor 2 catalyzed by fragment A from diphtheria toxin. Biochim. Biophys. Acta 483, 248–257 (1977).
Keen, J.H., Maxfield, F.R., Hardegree, M.C. & Habig, W.H. Receptor-mediated endocytosis of diphtheria toxin by cells in culture. Proc. Natl. Acad. Sci. USA 79, 2912–2916 (1982).
Mitamura, T. et al. Structure-function analysis of the diphtheria toxin receptor toxin binding site by site-directed mutagenesis. J. Biol. Chem. 272, 27084–27090 (1997).
Saito, M. et al. Diphtheria toxin receptor-mediated conditional and targeted cell ablation in transgenic mice. Nat. Biotechnol. 19, 746–750 (2001).
Jung, S. et al. In vivo depletion of CD11c(+) dendritic cells abrogates priming of CD8(+) T cells by exogenous cell-associated antigens. Immunity 17, 211–220 (2002).
Duffield, J.S. et al. Selective depletion of macrophages reveals distinct, opposing roles during liver injury and repair. J. Clin. Invest. 115, 56–65 (2005).
Clowes, A.W. & Schwartz, S.M. Significance of quiescent smooth muscle migration in the injured rat carotid artery. Circ. Res. 56, 139–145 (1985).
Clowes, A.W., Clowes, M.M. & Reidy, M.A. Kinetics of cellular proliferation after arterial injury. III. Endothelial and smooth muscle growth in chronically denuded vessels. Lab. Invest. 54, 295–303 (1986).
Savill, J. & Fadok, V. Corpse clearance defines the meaning of cell death. Nature 407, 784–788 (2000).
Sata, M. et al. Fas ligand gene transfer to the vessel wall inhibits neointima formation and overrides the adenovirus-mediated T cell response. Proc. Natl. Acad. Sci. USA 95, 1213–1217 (1998).
Pollman, M.J., Hall, J.L., Mann, M.J., Zhang, L.N. & Gibbons, G.H. Inhibition of neointimal cell bcl-x expression induces apoptosis and regression of vascular disease. Nat. Med. 4, 222–227 (1998).
Schneider, D.B. et al. Expression of Fas ligand in arteries of hypercholesterolemic rabbits accelerates atherosclerotic lesion formation. Arterioscler. Thromb. Vasc. Biol. 20, 298–308 (2000).
Sambrano, G.R. & Steinberg, D. Recognition of oxidatively damaged and apoptotic cells by an oxidised low density lipoprotein receptor on mouse peritoneal macrophages: Role of membrane phosphatidylserine. Proc. Natl. Acad. Sci. USA 92, 1396–1400 (1995).
Davies, M.J., Richardson, P.D., Woolf, N., Katz, D.R. & Mann, J. Risk of thrombosis in human atherosclerotic plaques: role of extracellular lipid, macrophage, and smooth muscle cell content. Br. Heart J. 69, 377–381 (1993).
Burke, A.P. et al. Coronary risk factors and plaque morphology in men with coronary disease who died suddenly. N. Engl. J. Med. 336, 1276–1282 (1997).
Bauriedel, G. et al. Role of smooth muscle cell death in advanced coronary primary lesions: implications for plaque instability. Cardiovasc. Res. 41, 480–488 (1999).
Kolodgie, F.D. et al. Localization of apoptotic macrophages at the site of plaque rupture in sudden coronary death. Am. J. Pathol. 157, 1259–1268 (2000).
Xu, W. et al. IL-10-producing macrophages preferentially clear early apoptotic cells. Blood (1996).
Acknowledgements
This study was supported by British Heart Foundation Grants PG/02/055/13778 and RG 04/001 (to M.R.B.); PG/05/127/19872 and PS/02/001 (to A.P.D.) and the European Vascular Genomics Network of Excellence (FP6).
Author information
Authors and Affiliations
Contributions
M.C.H.C. conducted and interpreted the majority of the experimental work and co-wrote the manuscript. N.F. performed the majority of the histological procedures. J.J.M. and A.P.D. conducted the contractile experiments and interpreted the data from them. M.G. advised on mouse pathology. T.D.L. and M.R.B. supervised and co-wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Fig. 1
Generation and characterization of transgenic mice. (PDF 133 kb)
Supplementary Fig. 2
Genotyping of Tgln2-HBEGF and Tgln2-HBEGF Apoe−/− mice. (PDF 901 kb)
Supplementary Fig. 3
Administration of DT induces VSMC-specific apoptosis in Tgln2-HBEGF mice. (PDF 92 kb)
Supplementary Fig. 4
Administration of DT does not induce nonspecific SMC loss in SM22α-hDTR mice. (PDF 170 kb)
Supplementary Fig. 5
VSMC apoptosis does not induce lymphocyte infiltration or expression of MCP-1/JE. (PDF 149 kb)
Supplementary Fig. 6
VSMC apoptosis induces vulnerable plaques in brachiocephalic arteries. (PDF 152 kb)
Supplementary Fig. 7
VSMC apoptosis increases serum IL-6. (PDF 82 kb)
Rights and permissions
About this article
Cite this article
Clarke, M., Figg, N., Maguire, J. et al. Apoptosis of vascular smooth muscle cells induces features of plaque vulnerability in atherosclerosis. Nat Med 12, 1075–1080 (2006). https://doi.org/10.1038/nm1459
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm1459
This article is cited by
-
Research Progress on Histone Deacetylases Regulating Programmed Cell Death in Atherosclerosis
Journal of Cardiovascular Translational Research (2024)
-
Transcription factors: key regulatory targets of vascular smooth muscle cell in atherosclerosis
Molecular Medicine (2023)
-
Vascular dysfunction caused by loss of Brn-3b/POU4F2 transcription factor in aortic vascular smooth muscle cells is linked to deregulation of calcium signalling pathways
Cell Death & Disease (2023)
-
Polo-like kinase 4 inhibitor CFI-400945 inhibits carotid arterial neointima formation but increases atherosclerosis
Cell Death Discovery (2023)
-
Agonist-induced Piezo1 activation promote mitochondrial-dependent apoptosis in vascular smooth muscle cells
BMC Cardiovascular Disorders (2022)